Don’t believe the misconception that post-traumatic stress disorder (PTSD) is just a mental issue that can be easily overcome. The reality is that professional treatment is often necessary for someone with PTSD to experience lasting recovery, regardless of how much support they receive from loved ones. If you’ve wondered What Is The Science Behind PTSD? We’re here to help. At Mind Flow Recovery, we understand the complexity of PTSD and provide comprehensive treatment to help people move forward in life. Our experienced professionals can work with you or your loved one to develop a customized care plan that best meets their needs and maximizes their chance of achieving post-traumatic growth. Discover how our innovative approach to effective PTSD treatment can open up the possibility for a meaningful journey.
What is Posttraumatic Stress Disorder?

PTSD Symptoms
The symptoms of posttraumatic stress disorder can vary from person to person but generally include the following:
- flashbacks
- sleep disturbances
- nightmares
- intrusive thoughts
- emotional numbness
- depression
- difficulty with concentration and memory
- hyperarousal or being easily startled
- avoidance of triggers and situations that evoke memories of the event(s)
- headaches
- fatigue
PTSD symptom severity can range from mild to severe and can last for months or even years. It is important to note that having PTSD does not mean one will have all of these symptoms.
Risk of Developing PTSD
There are a variety of factors that can increase the risk of someone developing PTSD. These include genetic predisposition, pre-existing mental health issues such as depression or anxiety, experiencing other traumatic events in the past, and personality traits such as being easily overwhelmed by stress. Other factors, such as a lack of support from family and friends, poverty, and substance abuse can also increase the risk of developing PTSD.
The Science Behind Post-Traumatic Stress Disorder
Research has shown that posttraumatic stress disorder is associated with changes in brain chemistry and brain structure. It’s believed that it results from a combination of biological, genetic, psychological, social, and environmental factors. To better understand how these changes occur, it helps to have a basic understanding of the human brain regions and their functions.
The Triune Brain Model
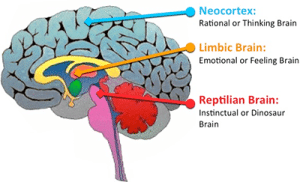
The second part of the triune brain is the limbic system, also known as the mammalian brain. This part of the brain is responsible for emotion and motivation. It’s believed that it plays an important role in the development of PTSD by helping to regulate emotions such as fear, anxiety, and aggression.
Finally, the third part of the triune brain theory is the neocortex or cerebral cortex. This part of the brain is responsible for higher-level cognitive functions such as language, problem solving, creativity, and abstract thought. It’s believed that trauma can cause changes in this part of the brain that affect memory and concentration.
Understanding Brain Regions
By understanding the different brain regions and their functions, it’s possible to gain a better understanding of how trauma can lead to posttraumatic stress disorder. Stress results in acute and chronic changes in the brain. It is believed that changes in certain areas of the brain can cause PTSD, including the amygdala and hippocampus.
Amygdala
Studies have found that those who experience post-traumatic stress disorder have an altered amygdala (the part of the brain that activates the sympathetic nervous system responsible for emotional processing) as well as reduced hippocampus size (the brain region related to memory and learning).
Studies have also found that trauma survivors have elevated levels of the stress hormone cortisol in their blood which can lead to physical and mental exhaustion, anxiety, and depression. Finally, research has shown that traumatic events are more likely to cause post-traumatic stress disorder if those affected lack access to sufficient social support following the event.
Hippocampus
The hippocampus is the part of the brain responsible for memory formation, and those with PTSD often experience difficulty forming new memories or accurately recalling events from their past. Research has suggested that trauma can lead to reduced hippocampal volume as a result of long-term activation of the stress response pathways in the brain which can interfere with normal functioning. These findings are supported by studies that have linked PTSD with decreased hippocampal volume, as well as changes in the hippocampus’s neural activity and connectivity.
Medial Prefrontal Cortex
The prefrontal cortex is a region of the brain responsible for planning, thinking, decision-making, and understanding emotions. Research has shown that in people with posttraumatic stress disorder (PTSD), the prefrontal cortex does not function as effectively as it does in those without PTSD. This means that survivors may have difficulty making decisions, controlling impulses, and modulating their emotions accurately in response to certain stimuli.
Studies have found that the prefrontal cortex is affected by hormones such as cortisol and adrenaline, which are released during times of stress or fear. It’s believed that this can lead to further disruption of the prefrontal cortex in those with posttraumatic stress disorder. The result is that people may experience difficulty controlling their emotions, concentrating on tasks, and managing their responses to stressors.
Cortisol Levels
Cortisol can trigger your fight or flight response by acting as a stress warning signal in your body. This hormone helps heighten alertness, but can also create feelings of fear and anxiety. Studies have found that people with PTSD have higher levels of cortisol in their blood than those without it. This suggests a connection between cortisol and the symptoms of post-traumatic stress disorder, such as difficulty concentrating, intrusive thoughts, flashbacks, and nightmares.
Ultimately, posttraumatic stress disorder is a complex disorder that is affected by both biological and environmental factors, but through evidence-based treatments such as cognitive behavioral therapy, individuals can learn to better cope with the symptoms. Through understanding the science behind post-traumatic stress disorder, those affected can better understand their own experiences and find the support they need to make a full recovery.
Overcoming An Overactive Amygdala
Fortunately, therapies such as cognitive-behavioral therapy (CBT) can help break this cycle. CBT is a type of talk therapy that helps individuals recognize and manage unhealthy thought patterns and behaviors related to their traumatic experiences. It encourages the individual to confront and accept their emotions while developing healthier coping mechanisms for stress management. Other types of therapeutic interventions, such as mindfulness-based practices, can also be helpful for those with an overactive amygdala.
Finally, it’s important to remember that the support of family and friends is invaluable in aiding a person with posttraumatic stress disorder to manage their symptoms. Those affected by PTSD must have access to help from professionals, but equally important is the emotional and psychological support of loved ones. With adequate care and understanding, individuals can eventually learn to manage their symptoms and live a fulfilling life.
Starting The Healing Process with Mindflow Recovery
Posttraumatic stress disorder is a serious condition that can have long-lasting effects. Fortunately, understanding the biology behind it and developing effective coping strategies can help those affected manage their symptoms and live a healthy life. It’s important to remember that everyone’s experience of PTSD is unique, so seeking professional help from an experienced mental health provider to find the best treatment plan for you is key. With the right care and support, individuals with PTSD can move forward in their healing journey and eventually achieve a sense of peace.
If you’ve experienced a traumatic event and are experiencing PTSD symptoms, it’s important to remember that you are not alone. Seeking professional help for mental disorders and the support of family and friends is the best way to start your journey toward recovery after experiencing trauma. Together, we can make a difference in how post-traumatic stress disorder affects individuals around us. You do not have to go through this alone. Help is available at Mindflow Recovery.
At Mindflow Recovery, we provide highly individualized, evidence-based treatment for individuals struggling with posttraumatic stress disorder. Our experienced and compassionate team of professionals will work closely with you to develop a comprehensive plan tailored to your unique needs. We understand that healing takes time, and we are here to assist you every step of the way. Contact us today to get started on your journey toward recovery from PTSD.
Treatment For Those Who Have Experienced Trauma

Through therapy, medications, lifestyle changes, and other interventions, those affected can find relief and learn to better manage their symptoms. With the right help and guidance, individuals with posttraumatic stress disorder can learn to live a life of balance and fulfillment.
Types of Therapies:
- Eye Movement Desensitization and Reprocessing (EMDR)
- Cognitive Behavioral Therapy (CBT)
- Dialectical Behavior Therapy (DBT)
- Exposure Therapy
- Acceptance and Commitment Therapy (ACT)
- Mindfulness-based Practices
- Medication Therapy
Eye Movement Desensitization and Reprocessing (EMDR)
A type of psychotherapy that helps individuals process traumatic memories. During EMDR sessions, patients are asked to recall their trauma while engaging in activities like eye movement, tapping, or auditory stimulation. This allows them to confront the memories without feeling overwhelmed or triggered and gradually releases the emotional charge associated with the trauma.
Cognitive Behavioral Therapy (CBT)
A type of talk therapy that helps individuals recognize and manage unhealthy thought patterns and behaviors related to their traumatic experiences. During CBT, patients learn to identify negative thoughts, challenge them, and replace them with more productive and healthy ones. This can help them confront their fears while building effective coping skills for managing stress.
Dialectical Behavior Therapy (DBT)
Dbt is an evidence-based approach that combines mindfulness, cognitive behavioral therapy, and dialectical strategies to help individuals regulate their emotions and behavior. It focuses on helping patients identify and accept their feelings while building effective coping skills for managing them.
Exposure Therapy
A type of psychotherapy that involves exposing a person to the traumatic memory or experience in a controlled setting. Through this type of therapy, individuals can learn to process and accept their fear while gradually gaining control over their reactions.
Acceptance and Commitment Therapy (ACT)
A therapeutic approach that encourages individuals to accept, rather than fight against, difficult thoughts and feelings related to trauma. This helps them learn to cope with their emotions without avoiding or suppressing them.
Mindfulness-based Practices
Mindfulness-based practices involve focusing one’s awareness on the present moment in a nonjudgmental way while observing thoughts and feelings without getting attached to them. This can help individuals become more aware of their emotions and regulate their reactions to trauma-related triggers. Mindfulness can also help build healthier coping strategies for managing stress.
Medication Therapy
In some cases, medication may be used to treat the symptoms of PTSD. For example, certain medications like selective serotonin reuptake inhibitors (SSRIs) can help reduce anxiety and depression associated with posttraumatic stress disorder. It is important to note that medication should only be used under the guidance of a qualified healthcare provider.
These types of therapies are designed to help those affected by PTSD develop a greater understanding of their emotional responses and learn strategies for managing symptoms. Through practicing these skills, individuals can ultimately find relief from the distress caused by posttraumatic stress disorder and live a life of balance and fulfillment.
At Mindflow Recovery, we understand that recovering from PTSD is a unique journey for each individual, which is why our experienced professionals will provide personalized treatments to help you reach your goals. We strive to create an environment of healing and support while helping you learn the skills needed for a successful recovery. Contact us today to begin your journey toward healing from PTSD.
Mindflow Recovery FAQ
Q: Why do some people develop PTSD but not others?
A: It is still not understood why some people develop posttraumatic stress disorder after a traumatic event while others do not. Research suggests that it may be due to a combination of genetic risk factors, environment, and individual history. People with certain pre-existing conditions or who have experienced multiple traumatic events are more likely to become affected by PTSD. The type of trauma itself can have an impact on the likelihood of developing posttraumatic stress disorder. Some people may be more resilient to certain types of trauma than others, while some may find it more difficult to cope with and process traumatic experiences.
Ultimately, each individual’s experience is unique, and their response to trauma will be different from that of another person. It is important for those who experience symptoms of post-traumatic stress disorder to seek the help of a mental health professional for proper diagnosis and treatment. With the right support, individuals can learn to manage their symptoms and move forward in their healing process.
Q: Can you prevent PTSD?
A: While it is not possible to completely prevent PTSD, certain strategies can help individuals reduce their risk. It is important for individuals who have experienced trauma to seek professional help if they are struggling with symptoms of post-traumatic stress disorder. Developing healthy coping mechanisms and engaging in self-care activities can also be beneficial in managing the impact of a traumatic experience. Additionally, having a strong social network of supportive people can help individuals build resilience and process their emotions. With the right support, individuals can make progress in managing their symptoms and gain control over their experiences.
Q: What are some strategies for managing PTSD?
A: There are various evidence-based treatments available that can help those with post-traumatic stress disorder manage their symptoms and live a life of balance and fulfillment. These treatments may include cognitive behavioral therapy, dialectical behavior therapy, eye movement desensitization and reprocessing, exposure therapy, acceptance, and commitment therapy, mindfulness-based practices, and medication management. Individuals need to work closely with their healthcare provider to develop a treatment plan that works best for them.
Q: Can you develop PTSD after a traumatic brain injury?
A: Yes, individuals with traumatic brain injury (TBI) can develop post-traumatic stress disorder. Research suggests that people who have experienced a TBI are at an increased risk of developing PTSD compared to those without TBI. If you or someone you know has experienced a TBI and is struggling with symptoms of PTSD, it is important to seek professional help. With proper treatment, people can learn to manage their symptoms and lead a life of balance and fulfillment.
Q: How do I know if I have post-traumatic stress disorder (PTSD)?
A: It is important to seek professional help if you are experiencing any of the following symptoms: recurrent intrusive thoughts or nightmares related to the traumatic event; flashbacks, feeling detached from your emotions or numbing them out; avoidance of traumatic reminders; irritability or difficulty sleeping; and increased anxiety or panic attacks. If you are experiencing any of these symptoms, it is important to reach out to a mental health professional for proper diagnosis and treatment. With the right support, individuals can learn to manage their symptoms and move forward in their healing process.